Find you way back…
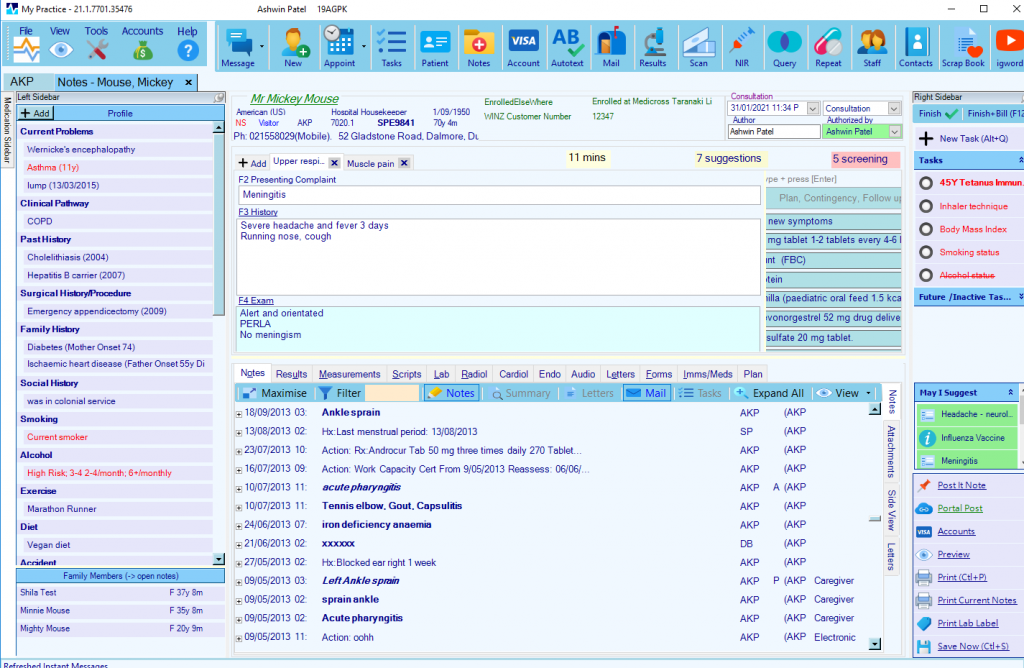
The Clinical Notes Screen
The clinical notes screen presents a SOAP template for you to enter consultation notes
You will see information around this central SOAP area that will provide context to this consultation
- The patient’s name and an overview of their demographic information appears at the top
- The problem list and risk factors are shown on the left (patient profile)
- Tasks (screening and recall jobs) appear on the right.
- The lower part of the screen displays a summary view of the patient’s recent encounters.
- The patients Medications and allergies can be included alongside the profile.
The time elapsed tells you how long you have spent with this patient so far.
A count of the patients waiting for you is updated every minute.
Problem Orientated SOAP notes
The presenting complaint
- Record the patients main reason for attending
History
- Enter the subjective history as obtained from the patient here
Examination
- Enter the objective findings of your examination here.
- Press F7 to enter measurements such as Blood Pressure, Weight, Height ….
Diagnosis
- Enter your working diagnosis or assessment here
- Press [Enter] to code this diagnosis
- Press [Tab] to skip the coding
- Change the colour of the diagnosis by using the colour drop down
- To control who can see or edit this diagnosis, set the security level in the dropdown next to the diagnosis code
- Author: Only visible to the original author
- Profession: visible to those with the same profession as the author
- Organisation: visible to those in the same organisation as the author.
- Private items are not included in referrals
- Hidden are not visible to casual on-lookers
Differential
Use this area to record other differential diagnoses being considered or ruled out. Click on the Differential link for suggestions for common symptoms.
Actions
(select left radio button)
- Type suggested actions or advice here then press [Enter]
- Enter as many actions as required.
- To remove an action, right click it and select Delete
Plan
(select right radio button)
- Record actions to be considered in the future here
Handing multiple separate problems
- To add another problem, click on the [+Add] tab
- Enter another SOAP note as above
- Return to any tab as required.
- Remove Problems and the associated notes by pressing the [X] on that tab.
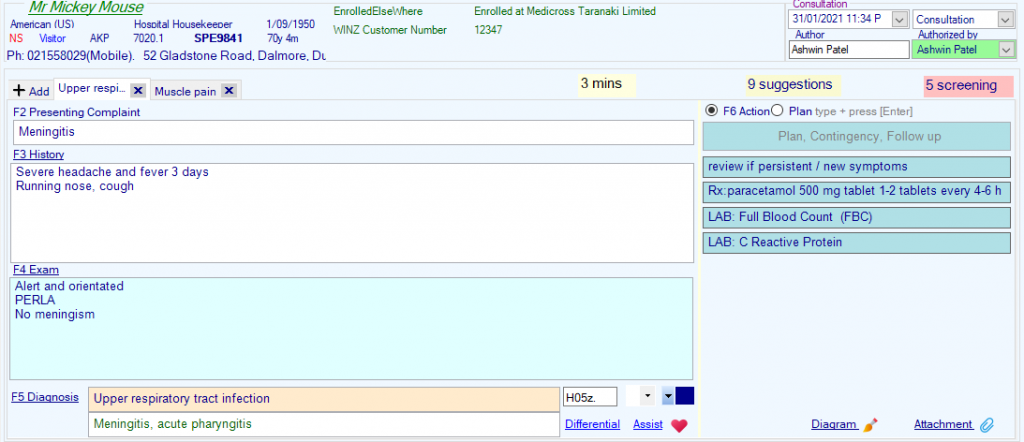
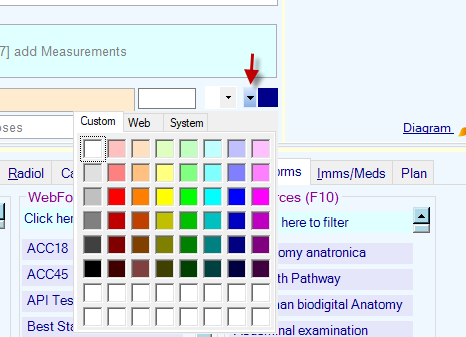
Include a diagram or an attachment
Draw on diagrams
- Click on the diagram link under the actions list
- Select from a list of templates with a BMP ending. (Popular diagrams include “Body Maps”, “Eye”,”Ear”)
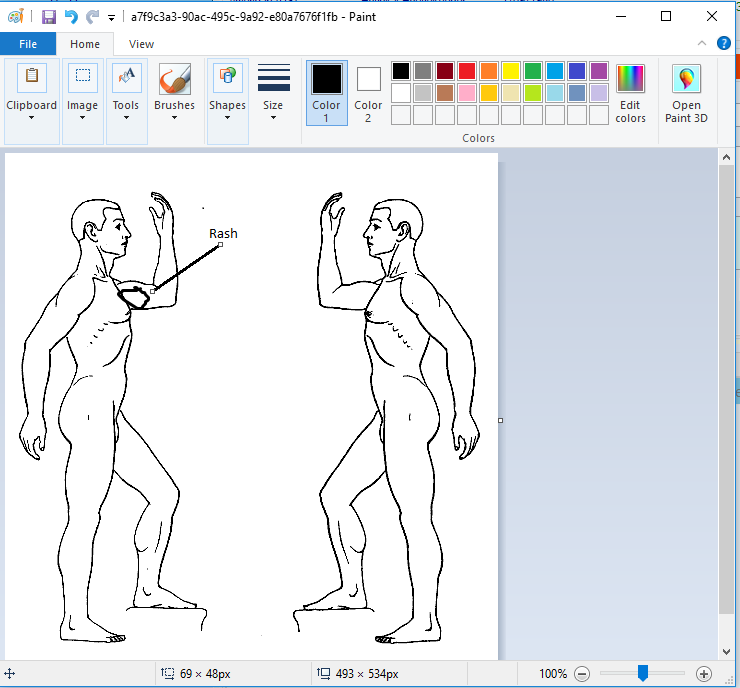
- Mark and annotate your diagram with Paint Tool
- Close Paint and choose Save Changes, providing a meaningful name .
Display educational diagrams
- Click on the diagram link under the actions list
- Select from a list of diagrams with a JPG or PNG ending.
- Close the picture tool when finished
Add an attachment
- Click on the attachment link
- Select a file from your computer or drive
- Update the filename when prompted
The original file will no longer be needed because when you attach a file it will be saved to the MyPractice database.
Using Assist
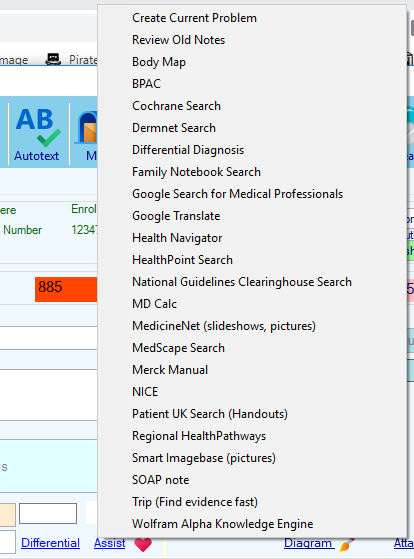
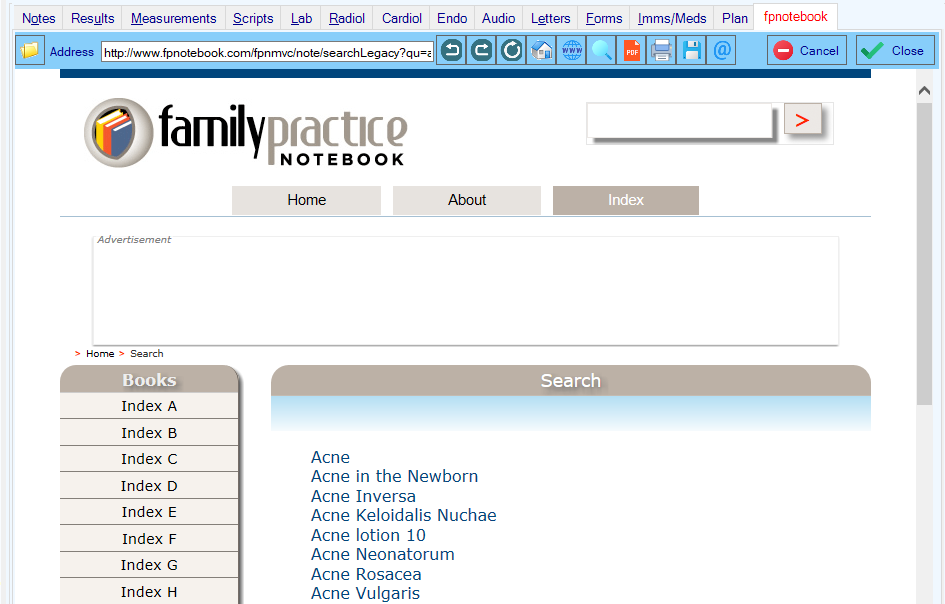
Click on Assist to see a list of websites that can help you make a diagnosis , get advice on treatment or educate your patient.
When you select a resource, it will open a website in a new tab.
The current diagnosis will be used to Search that website.
- These websites do not require subscriptions
- Click on the email button to send the website link to your patient
- Click on the Print button to print the website.
- Click on the PDF button to create a file of the webpage
- The Family Notebook provides up to date information in an easy to read note format
The Merck Manual provides comprehensive documentation - The Patient UK (NHS) provides great handouts for your patients
- The Smart Imagebase has pictures or videos on almost any condition
- MD Calc provides calculators and scoring templates
- Google Translate will find words in most languages
- Google search for Medical authorities – filters the sites professionally
Further sites are accessible in your resources list in the Forms Tab
When you are finished writing notes, review any overdue tasks then
- Click on Finish to save changes and print or send your forms and documents.
- Click on Finish + Bill to save changes and print or send your forms and documents then open the Billing screen.